Case Report
A Rare Neuroimaging of a Neurocutaneous Syndrome
4758
Views & Citations3758
Likes & Shares
Hypomelanosis of Ito (HI) is a multi-system disorder characterized by cutaneous, central nervous system, ocular and musculoskeletal defects. The cutaneous manifestations are very distinctive and help in identifying this disorder. We report a 9-year-old boy who presented with a constellation of clinical features that included skin hypopigmentation, nervous system abnormalities, skeletal deformity, heterochromia of the iris, facial, limb and corporal asymmetry. Magnetic Resonance Imaging (MRI) of the brain revealed hemimegalencephaly, hemimegacerebellum and periventricular heterotropia on the right side. The hemicorporal hypertrophy with cutaneous manifestations was found ipsilateral to the side of hemimegalencephaly. The typical phenotypical manifestations involving the entire neuroectoderm is exhibited in this case. The presence of hemimegacerebellum is very rare and has never been reported in association with this syndrome. Presentation of this case is to sensitize clinicians about this relatively uncommon disorder and to highlight the novel finding of hemimegacerebellum on imaging.
Keywords: Refractory epilepsy, Mental retardation, Neurocutaneous disorders
Abbreviations: EEG: Electroencephalogram; HI: : Hypomelanosis of Ito; MRI: Magnetic Resonance Imaging
INTRODUCTION
Hypomelanosis of ITO is a rare neuroectodermal syndrome with predominant neurocutaneous manifestations in the form of severe mental retardation, refractory epilepsy and hypopigmentation along the lines of Blaschko.
CASE REPORT
A nine-year-old male child was brought for evaluation of refractory seizures. He was born out of non- consanguineous marriage with an uneventful birth and family history. However, he had delayed milestones with significant learning disability. He started developing seizures of varied seimiology from 6 months of age (General Tonic Clonic Seizures, myoclonic jerks, head nodding and complex partial seizures).
Clinical examination revealed multiple dysmorphic features involving the skin, eye and skeletal system of which the cutaneous manifestations were striking. He had no dental anomalies. He had bizarre whorls on the right side of the trunk (Figure 1).
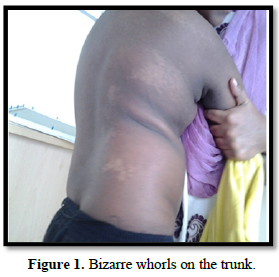

Bizarre whorls on the trunk which stopped short at the midline. He also had hypomelanotic areas over the right upper limb with loss of hair over the areas. His right lower limb revealed linear streak of hypopigmentation along the Blaschko Line (Figure 2).
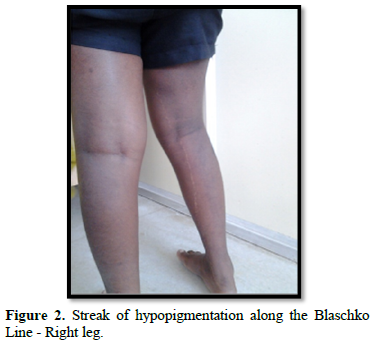

The face, scalp, palm and soles were spared of the hypopigmented skin lesions. All the skin lesions were present from six months of age. There was a gross asymmetry of the corpus, face and the limbs. He had heterochromia of right iris (Figure 3).
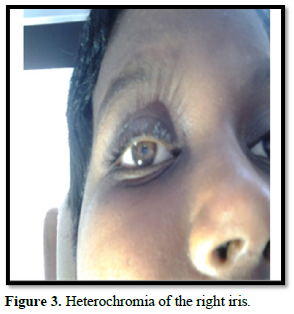

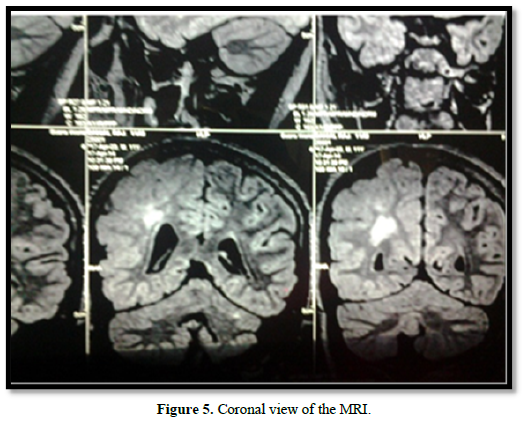
His right optic fundus revealed retinal pigmentary abnormalities. His musculoskeletal examination revealed kyphoscoliosis. The overall IQ of the patient was found to be 46, indicating severe level of intellectual disability. Spinomotor examination revealed subtle left hemiparesis. A complete metabolic, imaging and endocrine screening was carried out to rule out cardiac and renal defects. The brain MRI revealed FLAIR hyperintensities in the subcortical and periventricular region in the right hemisphere. The striking feature is the hemispheric asymmetry, ventricular asymmetry (right sided hemimegalencephaly with a thickened cortex and broad gyri), right ventricular heterotropia and right hemimegacerebellum (Figures 4 & 5).
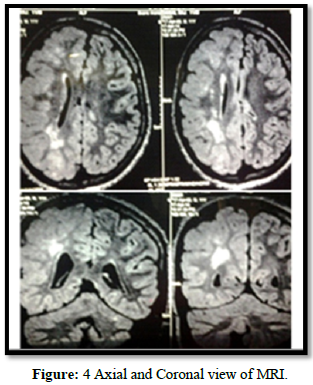


Electroencephalography revealed right left asymmetry with high amplitude slow waves over the right hemisphere.
DISCUSSION
Hypomelanosis of Ito (HI) is a neurocutaneous disorder. It is characterized by anomalies of the nervous, ocular, musculoskeletal, cardiac, renal and dental system in approximately 75% of the reported cases [1]. Our case had florid involvement of the neuroectoderm. The involvement of the Blaschko’s lines indicate the ectodermal cell migration pathways during the embryologic period. The cutaneous manifestations are usually found in all affected individuals and appear in the first year of life in 70% of cases [2]. In our case, it was noticed from 6 months of life. The entire spectrum of cutaneous manifestations from bizarre whorls to linear streaks were present with different patterns in different segments. The severity and area of involvement of skin changes may be widespread if the chromosomal mosaicism occurred early, whereas late onset may involve smaller regions [3]. The cutaneous manifestations on the upper limbs, trunk and lower limbs confirmed the involvement of three segments (cervical, dorsal and lumbosacral segments). The involvement of cutaneous lesions in three different segments helps to differentiate HI from congenital hypopigmented nevoid lesions which generally involve one segment only. Neurological manifestations reported were developmental delay (75%), moderate to severe cognitive deficits of IQ
CONCLUSION
The hemicorporal hypertrophy with cutaneous manifestations ipsilateral to the side of hemimegalencephaly is the typical phenotype exhibited with a novel finding of ipsilateral hemimegacerebellum. Presentation of the current case is to sensitize the clinicians about this relatively uncommon neurocutaneous disorder that can be diagnosed with meticulous clinical examination. The therapeutic efficacy of neurosurgical intervention for intractable seizures needs to be studied at large in these syndromic presentations. It is recommended that the General Practitioners and Physicians have low threshold to involve the multi-disciplinary teams as the management is predominantly conservative and symptom control. They may require support with speech & language therapy, occupational therapy, assessment of social circumstances and parental counselling.
- Glover MT, Brett EM, Atherton DJ (1989) Hypomelanosis of Ito: spectrum of the J Pediatr 115: 75-80.
- Pascual-Castroviejo I, López-Rodriguez L, de la Cruz Medina M, Salamanca-Maesso C, Roche Herrero C (1988) Hypomelanosis of Ito. Neurological complications in 34 cases. Can J Neurol Sci 15: 124-129.
- Lombillo VA, Sybert VP (2005) Mosaicism in cutaneous Curr Opin Pediatr 17(4): 494-500.
- Pascual-Castroviejo I, Roche C, Martinez-Bermejo A, Areas J, Lopez-Martin V, et (2005) Hypomelanosis of ITO. A study of 76 infantile cases. Brain Deve 20: 36-43.
- Oslon LL, Maria BL (2005) Hypomelanosis of Ito. In Singer HS, Kossoff EH, Hartman AL, Crawford TO Treatment of Pediatric Neurologic Boca Ranton Taylor & Francis pp: 561-564.
- Kalifa GL, Chiron C, Sellier N, Demange R Ponsot G, et al. (1987) Hemimegalencephaly: MR imaging in five Radiology 165: 29-33.
- Cieuta-Walti C, Lavoie É, Patenaude Y, Echenne B, Sebire G (2006) Hemimegacerebellum: A Report of One Neuropediatrics 37(S1).
- Peserico A, Battistella PA, Bertoli P, Drigo P (1988) Unilateral hypomelanosis of Ito with Acta Paediatr Scand 77: 446-447.
- Ardinger HH, Bell WE (1986) Hypomelanosis of Ito. Wood's light and magnetic resonance imaging as diagnostic Arch Neurol 43: 848- 850.
- Ruiz-Maldonado R, Toussaint S, Tamayo L, Laterza A, del Castillo V (1992) Hypomelanosis of Ito: Diagnostic criteria and report of 41 Pediatr Dermatol 9: 1-10.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Journal of Rheumatology Research (ISSN:2641-6999)
- Journal of Nursing and Occupational Health (ISSN: 2640-0845)
- Journal of Infectious Diseases and Research (ISSN: 2688-6537)
- Advance Research on Endocrinology and Metabolism (ISSN: 2689-8209)
- Journal of Otolaryngology and Neurotology Research(ISSN:2641-6956)
- Journal of Allergy Research (ISSN:2642-326X)
- BioMed Research Journal (ISSN:2578-8892)







